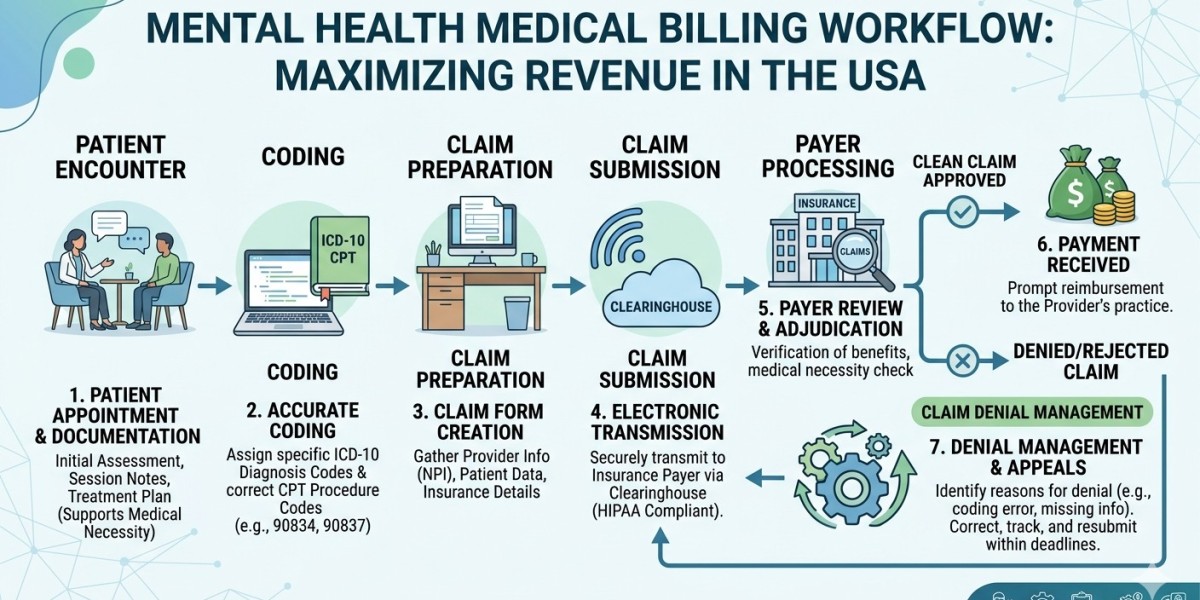
Mental health practices across the United States are growing rapidly, but so are the complexities tied to billing, coding, and insurance reimbursements. From ever-changing payer guidelines to strict compliance rules, providers often find themselves overwhelmed—not because of patient care, but because of administrative burden. This is where professional mental health billing services step in as a game-changer.
A well-structured billing system not only ensures timely payments but also improves cash flow, reduces errors, and enhances overall operational efficiency. Whether you are an independent therapist, a group practice, or a large behavioral health clinic, understanding how billing works is critical to your success.
Key Highlights of Mental Health Billing Services
• Accurate claim submission reduces rejection rates
• Faster reimbursements improve cash flow stability
• Compliance with insurance and federal regulations
• Efficient handling of coding and documentation
• Reduced administrative workload for providers
• Better patient experience with transparent billing
What Are Mental Health Billing Services?
Mental health billing services refer to the end-to-end process of managing claims, coding, submission, follow-ups, and reimbursements specifically for mental health providers. Unlike general medical billing, mental health billing involves unique coding structures, therapy session documentation, and insurance-specific rules.
These services cover everything from patient eligibility verification to final payment posting. When done correctly, mental health billing ensures providers get paid accurately and on time while maintaining compliance.
Why Mental Health Billing Is More Complex Than General Medical Billing
Mental health billing is not just about submitting claims—it requires deep knowledge of therapy-based services, time-based billing, and diagnosis-specific coding. Providers often face challenges such as:
• Frequent changes in insurance policies
• Strict documentation requirements for therapy sessions
• Time-based CPT coding complexities
• Limitations on session frequency and coverage
• Authorization requirements for treatments
Because of these factors, medical billing for mental health requires specialized expertise rather than a generic billing approach.
Core Components of Mental Health Billing
1. Patient Eligibility Verification
Before services are provided, verifying insurance coverage is essential. This includes checking co-pays, deductibles, and covered services to avoid claim denials later.
2. Accurate Coding
Coding and billing for mental health services rely heavily on CPT and ICD codes. Even minor errors can result in claim rejection or delays.
3. Claim Submission
Submitting clean claims to insurance companies ensures faster processing and minimizes denials.
4. Payment Posting
Tracking payments and reconciling them with claims helps identify discrepancies and underpayments.
5. Denial Management
Rejected claims are analyzed, corrected, and resubmitted promptly to recover lost revenue.
The Role of Coding in Mental Health Billing
Coding plays a critical role in mental health billing. Therapy sessions, psychiatric evaluations, and medication management all require precise coding. Errors in coding can lead to compliance issues or financial losses.
Coding and billing for mental health services demand expertise in time-based billing structures, such as 30-minute or 60-minute therapy sessions. Proper documentation must support these codes to ensure reimbursement.
Benefits of Outsourced Billing for Mental Health
Many providers today prefer outsourced billing for mental health instead of managing it in-house. This approach offers several advantages:
Reduced Administrative Burden
Providers can focus entirely on patient care instead of paperwork and billing complexities.
Improved Revenue Cycle
Professional billing teams ensure faster claim processing and fewer denials.
Cost Efficiency
Hiring and training in-house staff can be expensive. A cheap outsource mental health billing company can deliver better results at a lower cost.
Access to Expertise
Experienced billing professionals stay updated with industry changes, ensuring compliance and accuracy.
Choosing the Best Outsource Mental Health Billing and Coding Services
Selecting the right partner is crucial for long-term success. Here’s what to look for:
• Proven experience in mental health medical billing
• Strong understanding of payer guidelines
• Transparent pricing structure
• Advanced billing software and reporting tools
• Dedicated account management
The best outsource mental health billing and coding services not only handle claims but also provide insights to improve your revenue cycle.
Mental Health Billing and Credentialing Services
Credentialing is an often-overlooked but essential part of billing. Without proper credentialing, providers cannot receive reimbursements from insurance companies.
Mental health billing and credentialing services ensure that providers are enrolled with payers, maintain active status, and meet all compliance requirements. This directly impacts the ability to generate revenue.
Billing Medicare for Mental Health Services
Medicare billing comes with its own set of rules and guidelines. Providers must follow strict documentation and coding standards to avoid audits or penalties.
Billing Medicare for mental health services requires:
• Proper use of approved CPT codes
• Detailed documentation of therapy sessions
• Compliance with coverage limitations
• Accurate patient eligibility verification
Failing to meet these requirements can lead to claim denials or delayed payments.
Billing for Mental Health Therapists: Unique Considerations
Billing for mental health therapists involves additional nuances compared to other healthcare services. Therapists often deal with:
• Time-based billing codes
• Session documentation requirements
• Insurance pre-authorizations
• Out-of-network billing scenarios
Billing services for mental health therapists must be tailored to handle these specific challenges efficiently.
How Billing Services Support Mental Health Clinics
Billing services for mental health clinics go beyond claim submission. They help clinics scale operations by improving financial stability and reducing administrative workload.
Key advantages include:
• Streamlined workflow across departments
• Real-time financial reporting
• Improved patient billing transparency
• Faster reimbursement cycles
By outsourcing, clinics can focus on growth while maintaining a steady revenue stream.
Common Challenges in Mental Health Billing
Even experienced providers face challenges such as:
• High claim denial rates
• Complex payer requirements
• Incomplete documentation
• Coding errors
• Delayed reimbursements
Professional mental health billing services address these issues through structured processes and continuous monitoring.
Best Practices for Efficient Mental Health Billing
To ensure smooth operations, providers should follow these best practices:
• Maintain accurate and detailed documentation
• Verify insurance before every session
• Use updated coding guidelines
• Track claims regularly
• Address denials promptly
Implementing these strategies can significantly improve billing performance.
Future Trends in Mental Health Billing
The future of mental health billing is evolving with technology and policy changes. Key trends include:
• Increased use of automation and AI tools
• Growth in telehealth billing
• Stricter compliance regulations
• Value-based care models
Providers who adapt to these changes will have a competitive advantage in the industry.
Conclusion
Mental health billing is no longer just an administrative task—it is a critical component of a provider’s financial success. With increasing complexities in insurance policies and compliance requirements, relying on professional mental health billing services is becoming essential.
Outsourcing not only improves efficiency but also ensures accuracy, compliance, and faster reimbursements. Whether you are an individual therapist or a large clinic, investing in expert billing support can transform your revenue cycle.
Partnering with a trusted provider like 247 Medical Billing Services can make a significant difference. With expertise in medical billing services, medical coding services, medical billing and coding services, revenue cycle management services, and credentialing services, they help mental health providers streamline operations and maximize revenue without compromising patient care.
Frequently Asked Questions
What are mental health billing services?
Mental health billing services handle the entire billing process for mental health providers, including coding, claim submission, and payment tracking.
Why is mental health billing different from general billing?
It involves time-based coding, therapy documentation, and specific insurance guidelines that require specialized expertise.
Is outsourcing mental health billing a good option?
Yes, outsourced billing for mental health reduces administrative burden, improves accuracy, and increases revenue efficiency.
What is included in mental health billing and credentialing services?
These services include provider enrollment with insurance companies, compliance management, and billing operations.
How can billing services reduce claim denials?
By ensuring accurate coding, proper documentation, and timely claim submission, billing services minimize errors and rejections.
Do mental health therapists need specialized billing services?
Yes, billing for mental health therapists requires expertise in therapy-specific coding and insurance requirements.
What should I look for in a mental health billing company?
Experience, transparency, compliance knowledge, and strong reporting capabilities are key factors to consider.